Wound leakage with cataract surgery remains a challenge1
Even in a non-complex, single-plane Clear Corneal Incision (CCI) surgery, the rate of wound leak may be high1
A study* involving self-sealing CCIs for cataract surgery reported1:
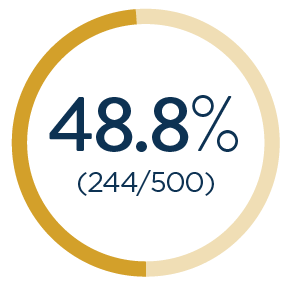
wound leak1

*A prospective, randomized, parallel-arm, controlled, multicenter, subject-masked study evaluated the safety and effectiveness of ReSure Sealant compared with a 10-0 nylon suture for preventing incision leakage from CCIs in patients having uneventful clear corneal cataract surgery after which a wound leak occurred. Patients scheduled for routine cataract surgery with no confounding ocular pathology were recruited. Patients were evaluated 1 hour after surgery and at 1, 3, 7, 14, 21, and 28 days. The primary endpoint was the percentage of eyes in which leakage occurred after treatment with ReSure Sealant or sutures in the 7 days after surgery.
Potential complications from wound leaks
Wound leakage can cause reduced intraocular pressure (hypotony).3
Hypotony can lead to vision-threatening complications, including:4
- Decreased visual acuity
- Choroidal detachment
44-fold increase in risk of endophthalmitis associated with leakage on postoperative Day 1.5†
Sutures can create additional risks6,7
- Induce corneal astigmatism
- Inflict tissue damage
- Cause vacuole formation in the corneal epithelium
- Increase the risk for endophthalmitis
- If suture removal is delayed, bacteria could be introduced into the anterior chamber
- 12.6% of eyes (23/183) in one study required earlier and unscheduled suture removal1*
- Removal on account of infection, foreign body sensation, conjunctival injection, astigmatism, or an elevated, loose, or broken suture
†A retrospective cohort study was conducted by chart review on patients who had cataract surgery at The John A. Moran Eye Center, Salt Lake City, Utah from January 1, 1996 to December 31, 2002. A 10% sampling (1525 charts) of all patients operated on for cataract surgery during this time period was compared to all cases of postcataract surgery bacterial endophthalmitis during the same time. Multivariate regression analysis was used to examine the development of postoperative endophthalmitis among study subjects based on study variables.
References: 1. Masket S, et al. J Cataract Refract Surg. 2014;40(12):2057-2066. 2. Masket S, et al. J Cataract Refract Surg. 2013;39(4):511-518. 3. Tong A, et al. Curr Opin Ophthalmol. 2018;29(1):14-18. 4. Sicco thoe Schwartzenberg GW, et al. J Cataract Refract Surg. 2001;27(4):549-554. 5. Wallin T, et al. J Cataract Refract Surg. 2005;31(4):735-741. 6. Nallasamy N, et al. J Cataract Refract Surg. 2017;43(8):1010-1014. 7. Shahbazi J, et al. Lasers Surg Med. 2011;43(6):490-498.
